One of the primary factors in determining and measuring the patient’s eligibility for noteworthy treatments is recording progress notes. These notes will greatly assist the mental health practitioner or psychotherapist to easily and quickly construct the progress of the patient’s treatment plan. With this method, it will save many hours of time-consuming paperwork. Are you studying to become a medical professional in psychotherapy? If yes, this article will be helpful for you in writing the progress note of your psychotherapy clients. So, we include some progress note templates to guide you in your medical service work. Keep on reading!
FREE 10+ Psychotherapy Progress Note Samples
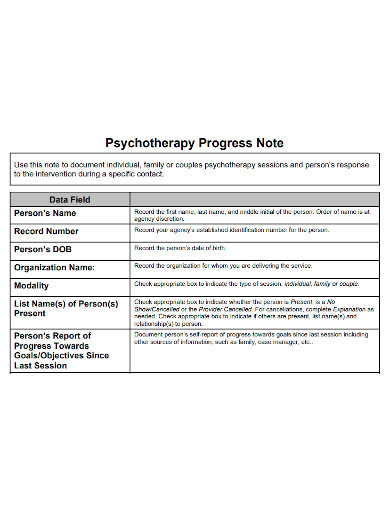
1. Psychotherapy Progress Note Sample
2. Medicare Psychotherapy Progress Note
3. Editable Psychotherapy Progress Note
4. Client Psychotherapy Progress Note
5. Printable Psychotherapy Progress Note
6. Standard Psychotherapy Progress Note
7. Patient Psychotherapy Progress Note
8. New Patient Psychotherapy Progress Note
9. Psychotherapy Progress Note Format
10. Adult Psychotherapy Progress Note
11. Psychotherapy Progress Note Planner
What is a Psychotherapy Progress Note?
Also known as a SOAP (Subjective, Objective, Assessment and Plan) note and a DAP (Data, Assessment and Plan) note, a psychotherapy progress note demonstrates a simple and comprehensible overview of each therapy session of the patient and a comprehensive record of the effects of the therapy to the child or adolescent psychotherapy patient.
Moreover, it is an essential document that comprises definite aims and objectives, as well as the whole development or entire progression of your client’s mental health or psychological therapy, rehabilitation for mental health due to drug and alcohol abuse, accidents, trauma, or any other circumstances.
How to Write a Psychotherapy Progress Note
While you eagerly work on facilitating several treatments for your psychotherapy clients, you also need to be able to write a structured and comprehensive progress report, DAP note or SOAP note of your clients to check and keep track their individual progress and show feedback to the clients and their guardians or parents about the progress in their therapy.
In this section, we give you some easy-to-follow tips that indicate how to design a comprehensive progress note for your patients:
1. Maintain a good therapeutic relationship with your patient
Use some helpful questions to ascertain and uncover what is inside the mind and heart of your client. You should think about maintaining a good therapeutic relationship with your client to promote change and further progress. Constantly review your method and respond to it.
Be determined and do your best effort when you show warmth and friendliness to your client. Make eye contact and allow time for small talk like a simple introduction. Then, ask your client about his or her problem.
2. Assess your patient’s needs
After initially discussing with your client, you can now create some assessment of your client’s needs. Research about the diagnosis you made according to his or her condition.
Take note of the methods and prescriptions that are crucial for your client’s therapy. Include all of this information to the client’s progress note as this will be the beginning phase of his or her progress of the treatment or therapy.
3. Elaborate the effects of the therapy
Then, after several weeks of the therapy, clearly elaborate in detail the effects of the therapy. Take note of the new symptoms that he or she is currently feeling due to the intake of some medications. If you notice that he or she needs to alter his or her psychotic medications due to some side effects, include this information on the progress note too.
Conduct some careful observations and diagnoses of your client for another week or even months, depending on his or her medical condition. Record every little bit of your client’s progress in your note and you may ask the client’s parents or guardians about his or her condition at home, at school, etc.
4. Use some psychological evaluation tests
Psychological evaluation tests or assessments are important tests that you need to conduct so that you are able to measure the progress of your patient. This series of tests is a beneficial tool in collecting information about how your clients think, feel, behave, and react. The findings are used as references to write a psychological report or a psychotherapy progress note of your client’s abilities and behaviors, as well as to be the foundation in making recommendations for his or her treatment.
FAQs
A psychotherapy progress note should include the patient’s symptoms, assessment, clinical diagnosis, treatments, failures and accomplishments, side effects of the treatments, etc.What should be included in a psychotherapy progress note?
The recorded notes are beneficial to the therapists because they can get back or review the essential details and noteworthy aspects of the therapy process, as they remember the recent accomplishments that were made by the patient and monitor the progress of the therapy. Why do therapists record notes?
Determine the main purpose and the nature of the daily progress report. Include some visual representations such as charts, graphs, tables, and diagrams. Keep in mind that your report should remain on topic or concept.How do you create a daily progress report?
A client’s psychological health records which include the psychotherapy notes must be kept by all licensed psychologists or mental health practitioners for a minimum of seven years from the discharge date of the patient or seven years after a minor patient becomes 18 years old. How long do I need to keep psychotherapy notes?
Therefore, writing a psychotherapy progress note for your client is a fundamental method in productivity management and maintaining organization in your job as a psychologist, psychiatrist, psychotherapist or mental health professional. Progress notes clearly demonstrate improvement in the client’s functioning, confirming that the client has made progress in his or her treatment. Also, take note that you must create and file formal amendments to the notes if you want to expand, delete, or otherwise change them depending on your clients or their families. Here are some of our downloadable and printable progress note samples available in different kinds of formats.
Related Posts
FREE 10+ Nurses Notes Samples in PDF
FREE 10+ Narrative Notes Samples in PDF
FREE 10+ After Interview Thank You Note Samples in PDF
FREE 14+ Money Promissory Note Samples in PDF
FREE 10+ Thank You Notes For Coworkers Samples in PDF
FREE 10+ Meeting Notes Samples in PDF
FREE 9+ Inpatient Progress Note Samples [ Psychiatric, Hospital, Complaint ]
FREE 10+ Note Taking Samples in PDF
FREE 10+ Credit and Debit Note Samples in PDF | MS Word
FREE 3+ Comprehensive Soap Note Samples in PDF
FREE 8+ Student SOAP Note Samples [ Medical, Pharmacy, Doctor ]
FREE 10+ Return Delivery Note Samples [ Product, Service, Electronic ]
FREE 3+ Car Sale Delivery Note Samples [ Transfer, Private, Vehicle ]
FREE 6+ Goods Delivery Note Samples [ Vehicle, Movement, Return ]
FREE 10+ Doctors Excuse Note Samples [ Office, Visit, Medical ]